Some Medicare drug prices will drop under new law, insulin co-pays to be capped
READ MORE
Figuring out Medicare
Medicare open enrollment runs from Oct. 15 through Dec. 7. Here’s what you need to know.
Expand All

As you turn 65, you must figure out Medicare — even if you plan to work beyond that
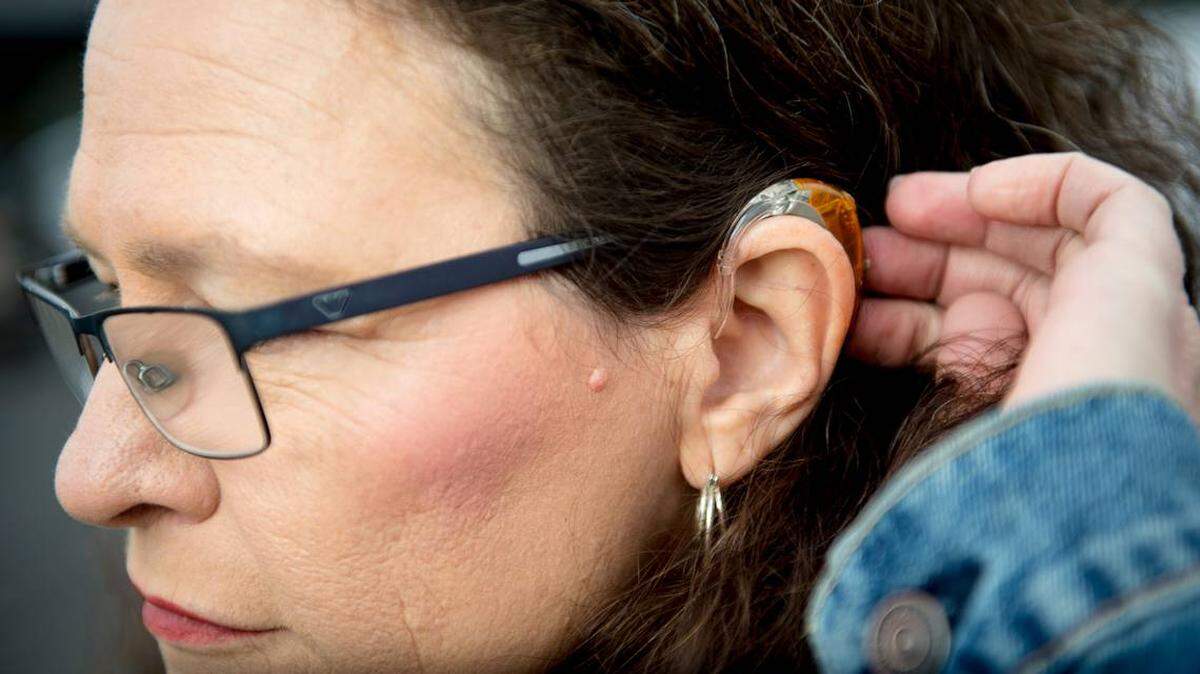
Medicare does not pay for everything — here’s how to fill in the gaps

‘It’s becoming too expensive to be alive.’ Seniors cope with soaring housing and food costs
Medicare Advantage plans — what you need to know before signing up in open enrollment
Some Medicare drug prices will drop under new law, insulin co-pays to be capped
In August, President Biden signed into law the Inflation Reduction Act (IRA) of 2022, aimed at lowering prescription drug prices for seniors.
One of the law’s key provisions is that the federal government will negotiate prices with drug manufacturers for certain drugs covered under Medicare Parts B and D, starting in 2026. Other measures call for drug companies to pay rebates if drug prices rise faster than inflation, cap out-of-pocket spending for Medicare Part D members and limit insulin costs.
“The Inflation Reduction Act is a sweeping piece of legislation that, in time, will have lots of significant impacts,” said Jeff Johnson, the State Director of AARP Florida.
“In terms of helping older Americans afford prescription drugs, once the IRA is implemented, Medicare beneficiaries will have the peace of mind that comes from knowing that the most they will pay for their medications through Medicare Part D is $2,000,” said Johnson.
“At the same time,” he said, “this law will help rein in price increases of prescription drugs, use the government’s power to negotiate with drug companies to lower prices, and cap insulin costs at $35 per month, among other things,” he added.
READ MORE: As you turn 65, you must figure out Medicare — even if you plan to work beyond that
Drug prices outpace income increase
The average cost of prescription drugs jumped by more than 26 percent a year between 2015 and 2019, compared with 15 percent annual income gains, according to the American Association of Retired Persons (AARP).
AARP research also showed that the average older American takes 4.7 prescription drugs a month and Americans pay two to three times more than other countries for the same brand-name drugs..
Timeline for drug price changes
The prescription drug measures included in the new law will be phased in over time.
Here’s a timeline of when the provisions will go into effect:
▪ In 2023, monthly insulin caps will kick in, along with rebates from drug companies if their prices go up faster than inflation. Co-pays for adult vaccines covered under Medicare Part D will be eliminated.
▪ In 2024, caps on out-of-pocket spending for Medicare Part D members take effect, as well as expanding Medicare’s low-income subsidy program.
▪ In 2026, the federal government will begin negotiating with drug manufacturers on the price of some drugs.
Here is what you need to know about key proponents of the law:
Insulin caps
Beginning in 2023, co-pays for a 30-day supply of insulin will be capped in Medicare Part D. This will benefit about 3.3 million Medicare beneficiaries with diabetes.
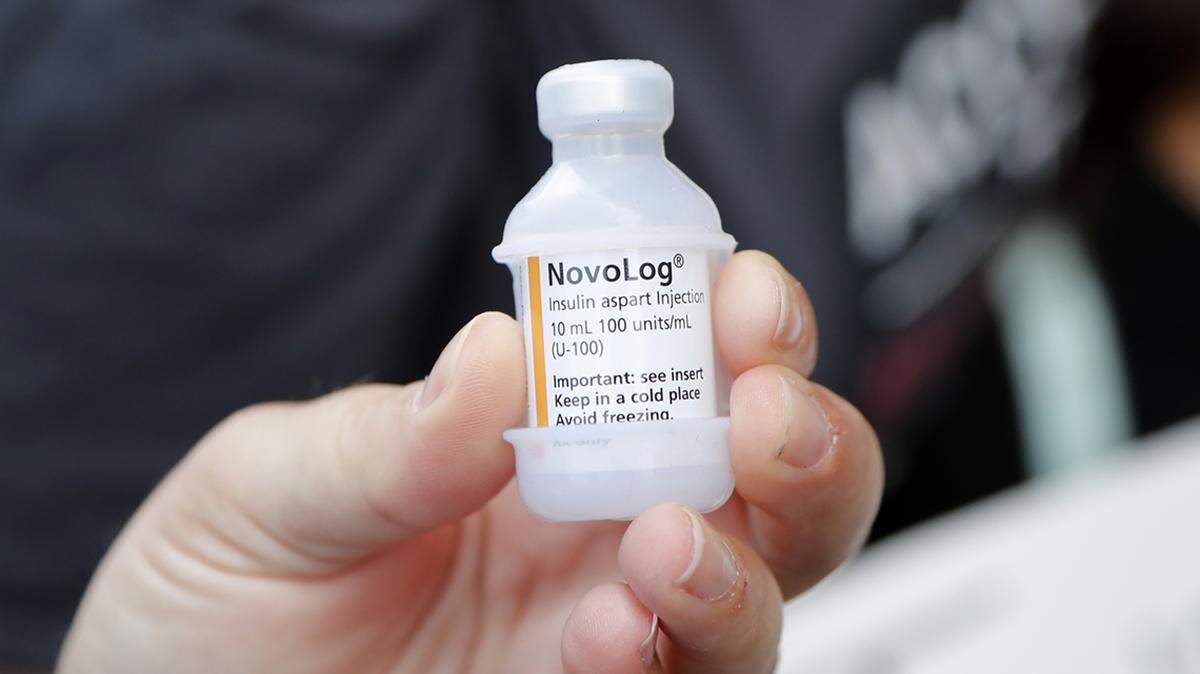
From 2023 to 2025, the maximum monthly co-pay will be $35. For 2026 and thereafter, the monthly cost will be $35 or 25% of the drug’s negotiated price, whichever is lower.
Part D plans will be required to offer this co-pay amount even before the enrollee meets their deductible for the year.
“There is a lot in this law, but the bottom line is that your bottom line, as a Medicare beneficiary, will finally see some relief,” said Johnson.
READ MORE: Deciding whether Medicare Advantage plans are right for you
What drugs are eligible for negotiation?
Not all drugs are eligible for price negotiation.
Tricia Neuman, director of the Program on Medicare Policy at the Kaiser Family Foundation, said the law excludes drugs from negotiations if they have a generic or biosimilar drug available.
“It also excludes drugs that are less than nine years from FDA approval (small-molecule drugs) or less than 13 years from FDA approval (biological products),” she said.
It also exempts drugs from certain small biotech companies, and drugs that are designated as “orphan drugs” as the only FDA-approved indication, she said. An orphan drug is defined as one “intended for the treatment, prevention or diagnosis of a rare disease or condition, which is one that affects less than 200,000 persons in the US,” according to the Food and Drug Administration.
All plasma-derived products are also exempt.
“The Secretary of Health and Human Services (HHS) is required to negotiate drug prices for a limited number of Medicare-covered drugs each year,” said Neuman.
The negotiated prices will apply to 10 drugs in 2026, 15 drugs in 2027, 15 drugs in 2028 and 20 drugs in 2029, she said.
Monthly Part D premiums
“It’s not exactly clear what this will mean for Medicare Part D premiums,” said Neuman.

She said that negotiated prices and inflation rebates are expected to reduce Medicare Part D drug spending, according to the Congressional Budget Office (CBO), which will put downward pressure on premiums.
“But the law also improves coverage under Part D by adding an out-of-pocket cap, and that could increase Medicare spending and premiums,” she added.
“Anticipating this uncertainty,” she said, “the law limits annual Medicare Part D premium increases to no more than 6 percent each year for the next several years.”
Out-of-pocket spending
“The biggest winners are likely to be Medicare beneficiaries who pay thousands and thousands of dollars for their drugs, even with Part D,” said Neuman.
The current Part D benefit does not have a hard cap on out-of-pocket spending, which means people who take expensive drugs for conditions like cancer and multiple sclerosis (MS) can face huge bills when they pick up their prescription, she said.
“There’s some evidence that even cancer patients go without medications prescribed by their doctors because they can’t afford it,” she added.
The new law will limit out-of-pocket spending on Part D to approximately $3,250 a year, beginning in 2024. The law also adds a hard cap on out-of-pocket spending to $2,000 in 2025.
“That still sounds like a lot to pay in a year, particularly for seniors living on modest incomes, but it is much less than some are paying today,” she said.
An estimated 1.4 million Medicare beneficiaries paid more than $2,000 for their prescription drugs in 2020.
Inflation provisions
The number of Medicare beneficiaries in Florida who will be impacted by the Inflation Reduction Act will depend on which drugs are chosen for price negotiation and which drugs have their prices rise faster than the rate of inflation, according to Emma Claire Boswell Dean, an assistant professor of Health Management and Policy at the University of Miami Herbert Business School.
“However,” said Dean, “we can expect the legislation to have broader impacts even outside the Medicare program.”
“For instance,” she said, “the inflation provision might affect the price at which drug manufacturers decide to launch their new products, which could impact costs even for patients who are privately insured.”
“Prescription drug manufacturers will be required to pay a rebate to Medicare if they raise prices faster than the rate of inflation,” she added.
She said that this would be the case for retail and specialty pharmacy drugs covered by Medicare Part D, as well as drugs that are dispensed by physicians, including infused drugs like chemotherapy, which are covered by Medicare Part B.
A lifeline for older adults
According to a statement from the White House, 5 to 7 million Medicare beneficiaries could see their prescription drug costs go down because of the provision allowing the federal government to negotiate prescription drug costs with drug manufacturers.
In addition, 50 million Americans with Medicare Part D will have their costs at the pharmacy capped at $2,000 per year. This benefits about 1.4 million beneficiaries annually.
“The IRA’s financial protections and structural improvements will be nothing short of lifesaving,” said Fred Riccardi, president of the Medicare Rights Center, in a press release.
“Every day on Medicare Rights’ national helpline, we hear from older adults and people with disabilities who are struggling to pay for care,” he stated. “They may go without, or may cut back on other basic needs, like food or rent, just to fill a prescription. The IRA will help ensure fewer people face these impossible choices.
The press statement also highlighted some of the bill’s shortcomings.
“We will continue to advocate for needed changes,” said Riccardi, “including those that were under consideration but ultimately left out of the bill, such as allowing Medicare Part B to cover comprehensive vision, dental, and hearing services; investing in Medicaid home- and community-based services; closing the Medicaid coverage gap; and streamlining the Medicare Part D appeals system.”
Low-income subsidy
The low-income subsidy extra help for Medicare Part D is another program that helps Medicare beneficiaries pay for prescription drugs. The program reduces or eliminates the Medicare Part D premium, deductible and co-payments for those who qualify.
A Medicare beneficiary can also have this subsidy if he or she is a member of a Medicare Advantage Plan.
“This low income subsidy extra help for Part D applies to both traditional Medicare and to Medicare Advantage Plans,” says Kathleen Sarmiento, who serves as the SHINE Medicare/Medicaid Counseling Program Director at Alliance for Aging in Miami-Dade County.
To be eligible, the Medicare beneficiary has to have a monthly income of less than $1,699 and assets (savings) of less than $15,510, she says. For a couple, the income qualifications are a joint monthly income of less than $2,289 and assets (savings) of less than $30,950.
“The home where the person lives and their automobile are not counted as assets when applying for these financial assistance programs,” Sarmiento added.
This subsidy is not a part of the Inflation Reduction Act.
“It has been in existence for a few years,” said Sarmiento, “although many people are not aware of it.”
The new law will expand eligibility for this program.
How to get help in selecting a plan
Sarmiento recommends that everyone on Medicare do an insurance comparison during the Medicare Open Enrollment Period from Oct. 15 to Dec. 7.
For a free and unbiased comparison of 2023 Medicare Part D plans or Medicare Advantage Plans or both, contact the Florida SHINE team at www.floridashine.org under the “Contact Us” tab.
Those who prefer to talk via phone can call 1-800-96-ELDER (1-800-963-5337) and ask for SHINE. In Miami and the Florida Keys, call 305-671-6356.
Appointments via telephone, Zoom and in-person are available. For a list of in-person sites, visit www.floridashine.org.
To contact Medicare by telephone, dial 1-800-633-4227.
“I also want to remind everyone that insurance agents from Medicare Advantage Plans (HMOs, PPOS, HMO-POS, SNP) and Part D plans are not allowed to call you or visit your home without a specific invitation from you,” said Sarmiento.
“If you receive an unsolicited call or visit from an insurance agent, please report it to SHINE,” she said.
“We all want to prevent Medicare fraud,” she added. “Treat your Medicare number like you would a credit card number — don’t give it out unless you want to change your insurance.”
This story was originally published October 15, 2022 at 5:00 AM.