Florida and Miami-Dade change plans to host hurricane evacuees in hotel rooms
Floridians facing an unprecedented storm season combined with a global pandemic may be more likely to evacuate to a hotel room than a friend’s house this year. But now, their options for getting the government to foot the bill are limited.
Florida’s plan to offer hotel rooms to anyone seeking an isolated place to evacuate from a hurricane has changed, according to guidance given to county emergency managers. Now the state plans to offer that option only to people who are COVID-19 positive, “knowingly” exposed to COVID, under quarantine orders, are older than 65 or have a pre-existing condition. Evacuees will get a hotel room and food covered for up to seven days via the Safer Florida app, which won’t be available for download until a storm is coming.
The state Department of Emergency Management did not respond to questions about the change.
Miami-Dade County, which was previously considering offering hotel rooms as evacuation spots, is also discontinuing those plans.
“After we started dealing with these hotels we scrapped the whole idea. It presented a multitude of problems,” said Frank Rollason, Miami-Dade’s director of emergency management.
There are only 34 hotels in the county that aren’t in evacuation zones, and the county had trouble determining which ones were strong enough to withstand major hurricanes.
There’s also the issue of food. The hotels told the county they weren’t going to be able to guarantee if their hotel would be open in the event of a storm, let alone their kitchen. Some of the prospective hotels don’t have interior hallways, and the lockable doors make monitoring for COVID symptoms or patrolling for security issues a problem.
“We’ve been through so many scenarios, and it’s another disaster waiting,” Rollason said.
Another plan from the state to make evacuating in a pandemic safer, rapid COVID testing, hasn’t materialized either.
“There was a lot of hope that by the time we got into the most active part of hurricane season we’d have rapid tests at scale,” said Craig Fugate, a former head of FEMA who was Florida’s emergency director during the infamous hurricane seasons of 2004 and 2005. “We just don’t have that.”
Instead, emergency managers are focused on protecting the options of last resort for hundreds of thousands of people: public hurricane shelters.
Shannon Weiner, director of emergency management in Monroe County, said implementing some of the new best practices for lowering the risk of COVID transmission should be simple for her small county. Monroe’s four shelters are all schools, so they’re expanding from just the auditorium to individual classrooms, with some set aside for COVID-positive people. That allows for the state-recommended 60 square feet per evacuee instead of the usual 20 square feet.
Weiner said evacuees will be screened for symptoms at the door, and a staffer will check everyone’s temperatures and screen for symptoms every 12 hours. The Department of Health is providing someone from the medical reserve corps for each shelter.
“They will be a safe place. Don’t be afraid to go. We work very hard to make them safe for you,” she said.
Miami-Dade will also screen for symptoms, separate potential COVID-positive evacuees and distribute masks and hand sanitizer within shelters. But the state’s most populous county can’t meet Florida’s recommended spacing of 60 square feet per evacuee forever.
When Tropical Storm Isaias was bearing down on Florida, Rollason said Miami-Dade had 20 shelters ready to open, compared to the eight it would have opened in non-pandemic times. The county has 82 available shelters to open this year.
“We’ve made the modifications we can, but if we get a big storm they’re gonna be packed in. There’s no other option,” Rollason said.
As storm-prone places around the nation grapple with a new set of rules for hurricane prep in a pandemic, there’s been little discussion on where, exactly, evacuees will go besides local shelters.
A new study from Columbia University and the Union of Concerned Scientists found that directing evacuees to counties with lower rates of COVID could lessen the spread of the virus in the wake of a storm. The study has not yet been peer-reviewed, which means fellow scientists have not checked to see if the research was sound.
The researchers looked at the evacuation patterns from 2017’s Hurricane Irma, where 2.3 million people evacuated from Monroe, Miami-Dade, Broward and Palm Beach counties, and modeled a 2020 evacuation that followed the same patterns.
But Kristy Dahl, report co-author and senior climate scientist at UCS, acknowledged that it’s not a perfect match. For one, Irma had a unique track up the middle of the peninsula, sending people fleeing from both coasts and going farther north to escape the storm. Also, in the COVID era, people are probably less likely to consider evacuating by plane as thousands did for Irma.
“It’s not necessarily a perfect analog for a storm approaching the Atlantic coast, but it’s the best available one,” she said.
The study considered a best-case and worst-case scenario for transmission. It found that if people stayed isolated while evacuating (as in, staying in individual hotel rooms or carefully rooming with family) there could be as few as 9,100 additional cases resulting from the evacuation. If everyone mingled or stayed in overcrowded shelters, researchers said there could be as many as 61,000 new cases.
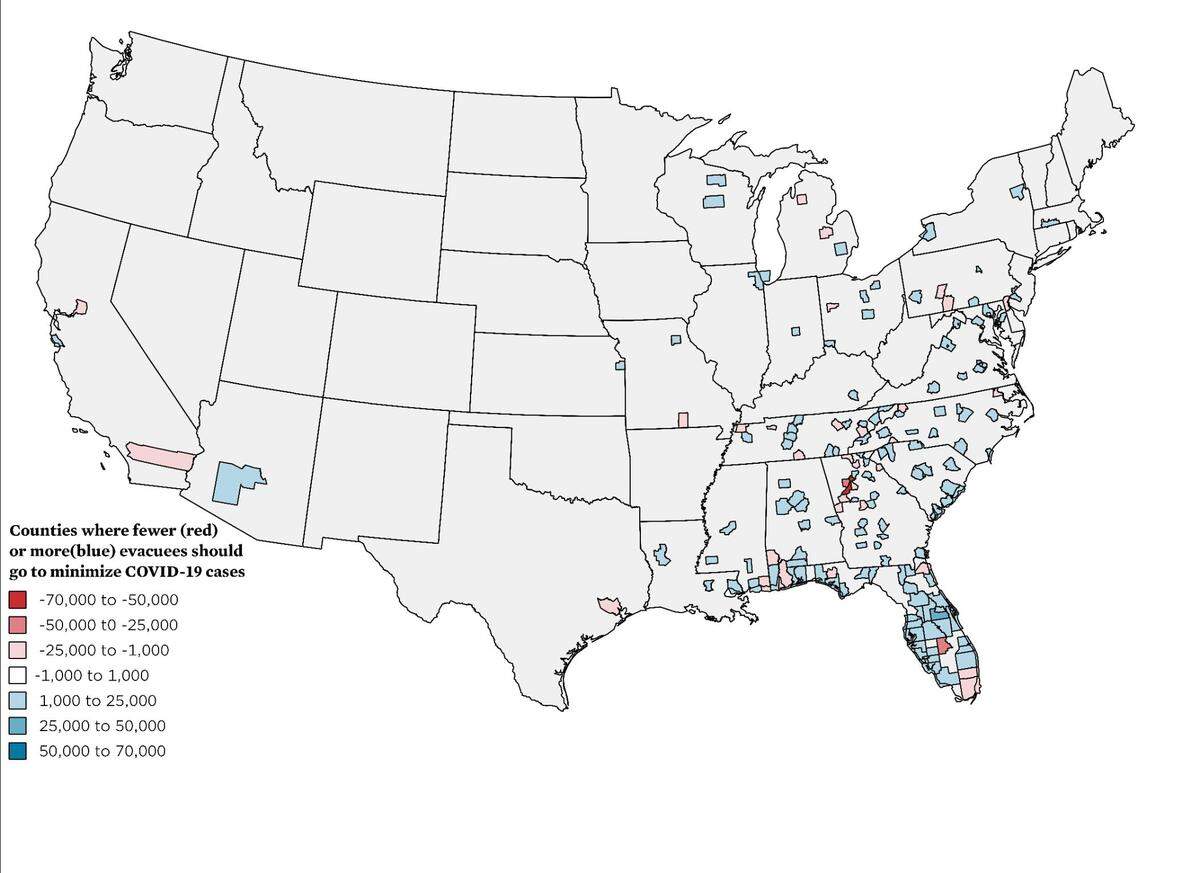
The scientists also found that directing evacuees to counties with low rates of COVID and away from counties with high rates could slow the spread of the virus. For example, Highlands County, which is just north of Lake Okeechobee, would need to take 27,000 fewer people. Orange County could take up to 48,000 more people.
However, emergency managers said the concept of directing people where to evacuate is rarely up to them.
“The reality is people follow roads, despite whatever guidance you give them,” Fugate said. “The traffic starts to take on a life of its own. Most people just drive to a location or stop when they run out of options.”
Rollason, of Miami-Dade, said counties occasionally ask to open shelters in “host counties,” but that usually involves carting in supplies and staff from the county doing the asking.
Plus, he said, people generally choose to stay with friends or family, or get a hotel, rather than go to a shelter. Studies have shown fewer than 10 percent of people choose a public shelter. Miami-Dade has the capacity to shelter 412,000 people out of a population of 2.7 million.
“The problem with that with the COVID now is that maybe those friends don’t want people coming into their home,” Rollason said. “So that’s an issue.”
Dahl also suggested that the number of people looking for public shelters could rise due to the mass unemployment caused by COVID shutdowns.
“You have a lot more people who are in financially precarious states. The cost of staying in a hotel for a couple of nights, gas, those costs can be a real deterrent for evacuating,” she said.
The idea that residents may weigh the potential of catching COVID at a crowded shelter against the imminent threat of an incoming storm is a major concern for emergency managers this year.
“You’re in more danger from rising water than you are from the COVID virus. Whatever you do, you’re better off getting out of there than you are staying,” Rollason said.
This story was originally published August 20, 2020 at 7:00 AM.
