Can a simple shot at the doctor lead to flesh-eating bacteria? Here’s how to stay safe
Mike O’Grady’s lower back was hurting so he went to his doctor to get a steroid shot.
A few days later, the 68-year-old Florida grandfather went on vacation with his wife, Kelli, in the Panhandle. The two swam in the Gulf just off St. George Island.
Soon after this seemingly routine dip into the waters in late May, O’Grady felt more pain. And something even more startling.
When an infection grew to the size of an inflamed, hot lemon inside one of his butt cheeks, “it was a sign something wasn’t right,” the Citrus County man told WCTV.

How necrotizing fasciitis gets in the body
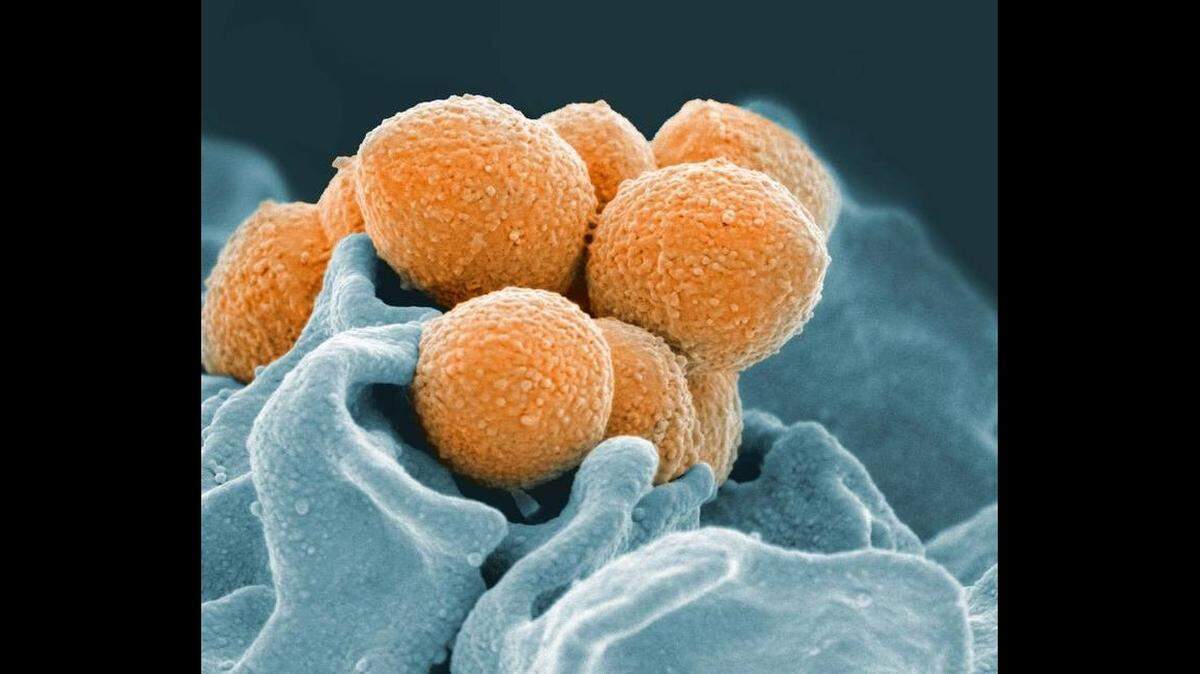
Doctors suspected necrotizing fasciitis, a bacteria that can live in warm waters, bays, pools, hot tubs and freshwater bodies. The bacteria, most often caused by the group A streptococcus bacteria, can enter the human body through cuts and scrapes, burns, insect bites, puncture and surgical wounds, according to the Centers for Disease Control and Prevention.
“It got in, possibly, most likely through this slight little tiny injection site where the steroids were put in,” O’Grady told WFTS ABC Action News. “The bacteria got in through those pinhole type injections,” O’Grady said.
As difficult as that is to imagine, that method of entry for the bacteria associated with staphylococcus or streptococcus infections are indeed possible, according to infectious disease experts.
“Where you find it is in little breaks if people are nicking themselves while shaving, and if the bacteria is there it can take advantage of the opening. Mosquito bites. Minute abrasions can be a point of entry,” says Dr. Gordon Dickinson, a staff physician at the Miami VA Healthcare System and professor of medicine at the University of Miami..
Blunt trauma that doesn’t puncture the skin can also allow the bacteria an entry point.
“If there is tissue damage, a little bleeding of any kind, if the bacterium are there they may see that area” as an entry, Dickinson said. Normally, that is handled by the body and cleared but if the person had a hemorrhage or tissue damage and have liver disease, the liver can’t clear the bacteria, he said.
“People with liver disease who eat seafood, particularly oysters, they may acquire” necrotizing fasciitis, said Dickinson, who did not treat O’Grady.
O’Grady told ABC Action News that he did not have any autoimmune issues.
Called ‘flesh eating’
Necrotizing fasciitis is often referred to as “flesh eating” for its voracious, and potentially fatal, appetite for human tissue.
“Necrotizing means causing the death of tissues. Fasciitis means inflammation of the fascia (the tissue under the skin that surrounds muscles, nerves, fat, and blood vessels)“ the CDC explains on its website.
Some health experts think climate change could be one factor for why people seem to be getting this bacteria after swimming in the Gulf.
“The trend will likely continue because of steadily warming temperatures in the Gulf of Mexico, which provide a ‘breeding ground’ for the bacteria, Dr. Sally Alrabaa, an an infectious disease specialist with USF Health and Tampa General Hospital, told The Tampa Bay Times.
Necrotizing fasciitis is still relatively rare, according to the CDC, which says there are about 500 to 1,500 cases reported annually in the U.S.
Flesh-eating bacteria was recently linked to the death of a Manatee County woman who sent swimming on Anna Maria Island, The Bradenton Herald reported.
O’Grady was more fortunate. He went through six days of surgery — which included an incision from his sternum to waist so surgeons at Citrus Memorial could inspect every inch of his digestive system for signs of necrotizing fasciitis — and 15 days of hospitalization.
O’Grady was released to recover at home on July 11, he said on Facebook. “Helluva way to lose weight,” one of his Facebook friends joked.
“I didn’t know how many friends I had before this happened,” O’Grady posted.
Precautions
Should you stop swimming in Gulf waters?
There are dangers in any activity, even walking around the house. Don’t live in fear, the UM’s Dickinson said. At the same time, take care if you’ve had something as seemingly innocent as an injection.
“If you have any obvious skin lesions, that should keep you out of Gulf waters during warm months,” Dickinson said. “If you have sores or lesions you should probably stay out of the water.”
The CDC also adds these suggestions:
▪ Clean all minor cuts and injuries that break the skin, including blisters and scrapes, with soap and water.
▪ Clean and cover draining or open wounds with clean, dry bandages until they heal.
▪ See a doctor for puncture and other deep or serious wounds.
▪ Wash hands often with soap and water or use an alcohol-based hand rub if washing is not possible.
▪ Care for fungal infections like athlete’s foot.
▪ Open wound or skin infection? Avoid hot tubs, swimming pools, natural bodies of water including lakes, rivers and oceans until wound heals.
Signs and symptoms
According to the CDC, signs of necrotizing fasciitis can include:
▪ A red or swollen area of skin that spreads quickly.
▪ Severe pain, including pain beyond the area of the skin that is red or swollen.
▪ Fever.
“See a doctor right away if you have these symptoms after an injury or surgery. Even though minor illnesses can cause symptoms like these, people should not delay getting medical care,” the CDC says.
Later symptoms of necrotizing fasciitis can include:
▪ Ulcers, blisters, or black spots on the skin.
▪ Changes in the color of the skin.
▪ Pus or oozing from the infected area.
▪ Dizziness.
▪ Fatigue.
▪ Diarrhea or nausea.
Treatment
▪ Prompt treatment is paramount.
According to the CDC: “Necrotizing fasciitis is a very serious illness that requires care in a hospital. Antibiotics and surgery are typically the first lines of defense if a doctor suspects a patient has necrotizing fasciitis. Since necrotizing fasciitis can spread so rapidly, patients often must get surgery done very quickly.”
This story was originally published July 26, 2019 at 10:22 AM.
