UM health system reports its ‘best financial year ever’ as cancer care and surgeries grow
The 560-bed hospital that once threatened to hang like a dead albatross around the neck of the University of Miami Health System has begun to show signs of a financial turnaround — inspiring talk of “a new day” from the chief executive for UHealth, the UM network of hospitals, clinics and doctors that make up the region’s only academic medical center.
“Last year, we had our best financial year ever,” said Dr. Edward Abraham, UHealth CEO.
A growing demand for cancer care, a rise in outpatient clinic visits and the consolidation of three separate UM hospitals under a single license helped UHealth record a $217 million profit for the year that ended May 31, according to a recent Securities and Exchange Commission filing.
That’s nearly three times the $83.8 million profit UHealth reported for the prior year, and includes some good news for the formerly named Cedars of Lebanon Hospital that UM purchased in 2007 but has struggled to make profitable in recent years.
Though the hospital, renamed UHealth Tower, lost $79.1 million for the year that ended May 31, there’s a silver lining: The loss is considerably less than the hospital’s prior year deficit of $94.5 million, and it does not account for a significant investment UM is making to refurbish the aging facility with new operating rooms, interior and exterior renovations, and infrastructure upgrades, including new generators and elevators.
UHealth announced in January that the hospital will be home to a new proton therapy program for cancer, which blasts highly charged proton particles at tumors, reducing damage to surrounding healthy tissue. The program is expected to debut in 2020.
Additional investments in UHealth Tower include five new cardiac catheterization labs and other resources aimed at rebuilding the hospital’s cardiac surgery program, which was set back by the November 2017 departure of two prominent surgeons, Donald Williams and Rogerio Carrillo, specialists in coronary bypass, valve repair, and aortic surgery.
Abraham declined to explain why Williams and Carrillo left UHealth. “I really can’t talk about the personnel actions,” he said.
The surgeons’ departure led to a reduction in cardiac surgeries at UHealth Tower over the past year, and the university has a strategy beyond investing in new resources to rebuild the program — recruiting a star physician who will attract patients from near and far.
Past and present UHealth executives familiar with the system’s plans said that star physician is Joseph Lamelas, a Cuban-American native of South Florida who is considered a pioneer in minimally invasive heart surgery. The former chief of cardiac surgery for Mount Sinai Miami Beach, Lamelas left South Florida for Baylor College of Medicine in Houston in 2017. Sources said he will return to Miami to work for UHealth in January.
Asked about Lamelas, Abraham blushed and laughed. “I can’t say anything,” he said.
The investments in UHealth Tower and the addition of Lamelas are designed to leverage two lucrative services for South Florida hospitals — cancer and cardiac care — and to enhance the system’s core brand as an academic medical center with a faculty practice of nearly 1,300 physicians and specialists, a medical school that trains doctors and performs research, and an integrated network of hospitals and clinics.
“It’s really our destiny,” Abraham said, “to set up these destination programs, these marquee programs that take full advantage of this expertise.”
But some hospital and healthcare experts doubt that UHealth’s brand as an academic medical center will be enough to set it apart from other health systems in the region that have made similar investments.
Baptist Health South Florida, the region’s largest nonprofit hospital system, opened a $430 million cancer center in January 2017 that is partnered with the nationally regarded Memorial Sloan Kettering Cancer Center in New York while Memorial Healthcare System in South Broward is partnered with Tampa’s H. Lee Moffitt Cancer Center and Research Institute, the state’s only National Cancer Institute-designated program.
Allan Baumgarten, an independent healthcare analyst and author of the bi-annual Florida Health Market Review, said lucrative lines of business for hospitals and health systems are also highly competitive.
“At a certain point,” he said, “you have to think that there’s a saturation point.”
Baumgarten said hospitals with destination cancer programs also are vulnerable to changes in payment by Medicare, the national health insurance program for Americans 65 and older, and the largest payer of hospital care in the United States.
Healthcare systems that deliver chemotherapy and other cancer treatment through outpatient clinics are allowed to charge hospital prices, which are higher. But Medicare is moving toward so-called site-neutral payments that would cap reimbursement for clinic visits at a lower rate comparable to that paid for care delivered in a doctor’s office.
“If Medicare is able to do that,” Baumgarten said, “then private insurers will likely follow.”
Joshua Nemzoff, a Pennsylvania hospital consultant who used to live in Miami, said UHealth must find a way to differentiate itself in a market where so many other hospitals and health systems offer more modern facilities located closer to where people live — and the quality of care is generally very good.
“There is no clear standout,” he said of South Florida hospitals.
That leaves UHealth with a small category of medical conditions in which to differentiate itself based on quality and expertise, such as trauma care and organ transplants, both of which are performed by UHealth doctors at Jackson Memorial Hospital.
“Heart transplants, kidney transplants, proton beam and brain surgery, that’s the kind of stuff. They can market that,” Nemzoff said. “Trying to say their heart surgeons are better than Baptist heart surgeons because they’re University of Miami, good luck. Everyone in the country has tried that at some point if they’re an academic medical center, and that’s just a very hard sell.”
Growth is also a challenge for UHealth because its competitors are not slowing down, said Baumgarten, the healthcare analyst. Large nonprofit hospital systems such as Baptist Health and Cleveland Clinic Florida are acquiring community hospitals and bringing more patients into their networks.
Baptist Health, the largest nonprofit hospital system in South Florida with 10 hospitals and more than 100 outpatient and doctors offices from Palm Beach County to the Florida Keys, recently signed a strategic affiliation agreement with Boca Raton Regional Hospital. And Cleveland Clinic Florida recently announced that the Indian River Medical Center in Vero Beach would join its network.
“The reason they’re doing that is they want to maintain and expand their patient access to their facilities and their specialists,” Baumgarten said. “They’re ... snapping up the community hospital feeders to the systems that provide the high-end specialty care.”
Abraham said his executive team is looking to form affiliations and joint ventures and possibly increase its longtime partnership with Jackson Health System, the taxpayer-owned hospital network for Miami-Dade County, with which UHealth co-brands a network of urgent care centers.
In healthcare, where technology and policy changes can occur suddenly, affiliations and acquisitions among hospitals require quick decision making. For UHealth, those decisions require the approval of the University of Miami Board of Trustees, which some past executives have criticized as being slow to act and lacking healthcare expertise.
Over the past decade, UHealth’s patient care operations have grown to make up more than 50 percent of UM’s $3.2 billion in annual revenues, including tuition, research grants and contracts.
Abraham says the university’s long-term strategic plan includes a proposal to spin off UHealth as an independent nonprofit; the short-term answer has been creating a UHealth advisory board stocked with healthcare professionals.
The UM Board of Trustees retains the authority to approve or deny big moves for UHealth, such as a merger, but Abraham expects the advisory board will allow the healthcare system to be more nimble.
“The intention is really to delegate major decision-making responsibilities to this board,” Abraham said. “There still will be the approval process through the University of Miami trustees, but they’re going to rely on the expertise of this board.”
Nemzoff, the Pennsylvania hospital consultant, said he doubts that UM trustees would willingly give up control of the biggest part of the enterprise.
“What you’ve got is you’ve got a very, very large healthcare system that happens to own a university,” he said. “The only reason you would spin off your healthcare system would be if you were concerned it was going to take down your university and you just didn’t want to have that risk.”
For now UHealth is benefiting from changes at the nearly $2 billion-a-year healthcare system, including a consolidation of facilities in November 2017 that helped to streamline finances and to unify electronic medical records and administrative policies.
The system’s three hospitals — Bascom Palmer Eye Institute, Sylvester Comprehensive Cancer Center, and UHealth Tower — consolidated under the license for Sylvester, which is designated by federal healthcare regulators as a so-called PPS-exempt hospital.
The special exemption applies to only 11 cancer hospitals in the country and affects Medicare payments to those institutions, reimbursing them at a rate that is, on average, about 42 percent more per patient than Medicare would have paid other local hospitals for providing cancer care, according to a 2015 report from the U.S. Government Accountability Office.
Under the consolidated license, the university has dedicated two floors at UHealth Tower to treat more cancer patients because Sylvester, which is across the street from the hospital, has only 45 beds.
“We absolutely needed a bigger facility,” Abraham said, “because cancer has been growing. Our bone marrow transplant services, our services for solid tumors, other oncology services are growing. The number of surgeries we’re doing for cancer are growing as well.”
Abraham said the hospital is not reducing other services to make room for cancer care. Part of the university’s $110 million investment to refurbish UHealth will fund a five-story addition. But he said UHealth is considering moving some services, such as behavioral health, out of UHealth Tower and into other inpatient settings.
PPS-exempt status carries another benefit for UHealth Tower. Those hospitals are excused from financial penalties imposed under Medicare’s Hospital Readmissions Reduction Program, which docks a percentage of all Medicare payments to hospitals with high rates of patients who are readmitted within 30 days after discharge for certain conditions, such as heart attack and pneumonia.
In the year before UHealth consolidated the licenses under Sylvester, UHealth Tower paid a readmissions penalty of three-quarters of 1 percent of all Medicare payments.
Abraham declined to say how much the hospital’s readmissions penalty amounted to in 2017. But he noted that consolidating hospitals under Sylvester’s PPS-exempt license also caused a reduction in Medicare reimbursement for other types of care, such as ophthalmology.
Overall, though, Abraham said, “There was expected to be revenue enhancement with single license, and indeed there has been.”
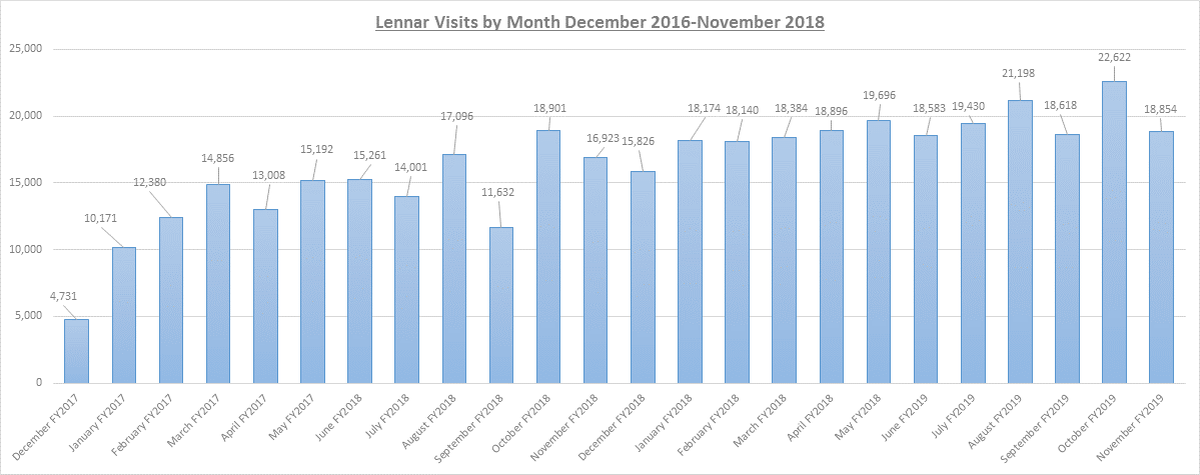
But he emphasized that healthcare systems are complex enterprises, and that many factors contribute to revenue growth, including the success of the Lennar Foundation Medical Center — a five-story, 26,500-square-foot outpatient clinic that provides a smorgasbord of care, from infusion and physical and radiation therapy to surgery, diagnostic imaging and ophthalmology at the UM campus in Coral Gables.
The ultra-modern outpatient Lennar Center, which features music, art and 200 hand-blown glass ibises in the entry, opened in December 2016. And rather than siphon business from UHealth Tower, the center has brought more patients into the UHealth system, Abraham said, citing a 13 percent increase in patient visits for 2018 over the prior year.
“It’s just doing fabulously well in terms of clinic visits,” he said, “but also in terms of patient experience.”
While Abraham acknowledges the difficulty of competing in South Florida’s healthcare market, he said UHealth is also trying to distinguish itself by treating its employees better. As an example, he said a recent compensation survey showed that salaries and benefits for UHealth nurses were competitive for the region.
After a series of layoffs at the hospital, and a raft of executive turnover at UHealth, Abraham said he is as focused on treating employees well as he is on financial performance because both are part of the equation for ensuring patient satisfaction.
“Culture here is a major issue for me,” he said. “How do we make sure that this is a uniquely good place for people to work?”
This story was originally published December 19, 2018 at 8:08 AM.
