They help COVID patients regain their basic skills — from sitting up to teeth brushing
After weeks or sometimes months in bed in an intensive care unit with a breathing tube down their throats, patients find that even the simplest tasks — like rolling over, sitting up, or brushing teeth — can be a struggle as they recover from the most severe cases of COVID-19.
Warren Graham was one of those patients. After a return flight from Jamaica where he suspects he may have contracted the virus, his wife drove him to Memorial Hospital Miramar when he began experiencing severe diarrhea. She would not see him again face-to-face for more than two months.
When he was stable and cleared of COVID, Graham was transferred to Memorial Regional Hospital South, the primary rehabilitation hospital in the Memorial system, in early April. He was in a wheelchair, and his left side was very weak. Although Graham had doubts about how quickly he would progress, within a week he could use a walker.
And on April 16, aided by daily sessions with occupational therapist Samuel Chege, Graham was released from the hospital into the arms of his family.
While doctors and nurses have saved lives during the pandemic, physical and occupational therapists have played a crucial role in helping COVID patients regain their independence and quality of life.
But some of them have gone well beyond what might be expected, helping not only their patients but the patients’ families and their hospital colleagues as well.
Chege, who was born in Kenya and has worked as a therapist for more than three decades, is among those therapist heroes.
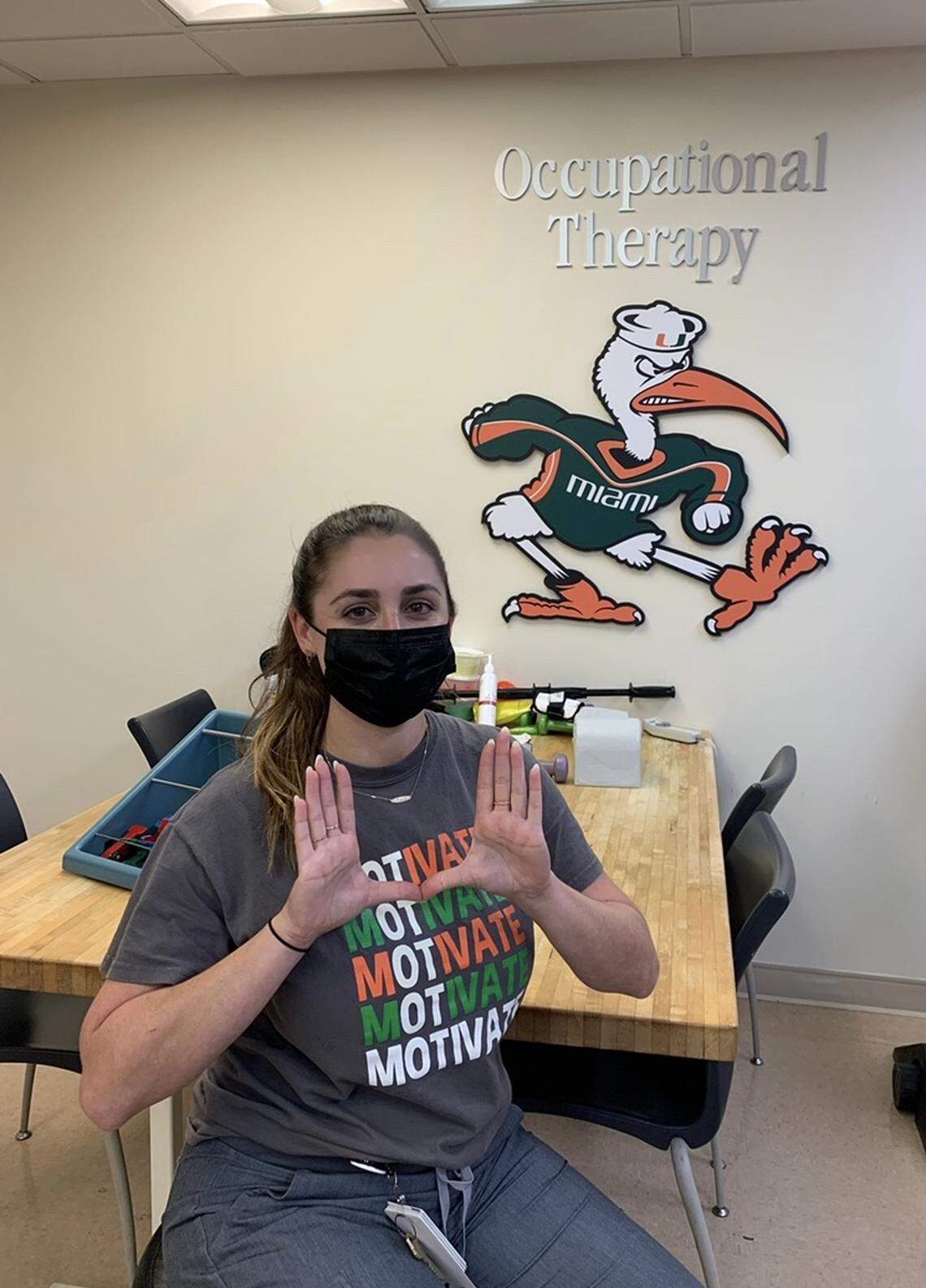
So is Danielle Rapaport, an occupational therapist who worked for nearly a year with COVID patients at UHealth — the University of Miami Health System and reached into her own pocket to buy supplies she thought would lift patients’ spirits and help provide a semblance of normalcy.
She not only worked with stiff and weakened limbs and joints, but also brought in hair detanglers and combs so that patients whose hair had become hopelessly matted after long periods in bed would start to feel human again. Rapaport brought a razor for a prickly patient whose hair and beard had grown long during his hospitalization and saw how just shaving his beard and head transformed his mood.
_A.jpg)
Cleveland Clinic Weston’s Tracy Smith is a hero, too. The director of physical therapy started a novel program to help stressed-out and overtaxed medical colleagues relax and get some self-care during the pandemic.
Working with COVID patients requires an understanding that their challenges during recovery aren’t just physical. Patients worry about their finances; they don’t want to be a burden on their families and ask for help with tasks they once did with ease, and their self-esteem after their ordeal is sometimes low.
Chege understands “the unique needs of patients who have been cleared of COVID-19, yet are dealing with weakened bodies, mind and spirit,” said Becky Boyle, his boss and the director of rehabilitative services at the hospital.
“Samuel’s goal is to get his patients to their highest functional level to be able to be reunited with their families and go home. He is compassionate, particularly with patients who have been in isolation for many days and weeks.”
’Just eating makes them tired’
“It’s such a big effort to do even the most basic things, like brushing their teeth, for many of them. Just eating makes them tired,” Chege said. Some patients are barely able to talk when they begin their therapy, he said.
Things that used to be easy like putting on clothes, washing and grooming and going from bed to a chair or to the toilet can be an ordeal, Chege said.
“When they go home, we want them to be able to do all these things for themselves if these were tasks they were doing before their hospitalization,” Chege said. “We want them to be functional to the highest level possible. Once I see they’re mastering one thing, we have to go to a higher level.”
He also likes to keep patients’ families abreast of their successes and allow them to ask questions, so he frequently does video chats when he is working with patients.
Chege said he has often heard patients say: “It seems like I won’t be able to do anything when I get home.” In addition to strengthening and flexibility exercises, “I need to encourage them and show them that they are making progress and taking small steps,” he said.
Some patients, especially those who have suffered strokes during their hospitalizations, may require home assistance so they don’t lose their balance and fall, but the goal is to get them to do as much of their personal care as possible, “relieving the burden on family members,” Chege said.
Graham, who is 54 and lives in Miramar, was one of the patients who had concerns he wouldn’t be able to handle basic tasks at home.
“It was very difficult for him initially. But now he’s really doing very well. I’m teaching him techniques for saving energy, so he doesn’t get so tired,” Chege said shortly before Graham was released from the hospital.
“He knows his stuff. Chege is a reliable, dedicated man who cares about his patients,” Graham said. “It’s not been easy, but I work hard because I want to get better. I was a little frustrated at the beginning, but I had to listen to Chege and do what he said, and he brought me around.
“I’m getting there one day at a time” thanks to Chege and the power of prayer, Graham said.
“For me, the biggest satisfaction is seeing patients who initially can’t care for themselves and are discouraged and then after a few days they are able to do a task they couldn’t do before,” Chege said. “When you see that, it just brings the greatest satisfaction.”
UM’s Rapaport says the role of an occupational therapist should be “figuring out what patients need — whatever is important to them” to restore them to their pre-COVID selves.
Detangling patients’ matted hair
For Rapaport, that includes helping them with their personal grooming until they are able to do such tasks on their own. One of her projects has been taming the bed head of patients whose hair has become tangled after spending lengthy periods in bed.
Armed with detangling combs and products, she says she has “saved a couple of women from having to have their heads shaved” because their hair had become so matted. “They call me the hair police,” she said with a laugh.
Rapaport has also helped patients FaceTime their families, played music for them on her phone, and arranged a “dance party” for a husband and wife who were hospitalized in adjacent rooms: “We opened the doors and helped get the wife in a standing position for the dance and we also positioned their chairs so they could see each other and ‘eat together.’”
Although she said some COVID patients are so sick they’re barely aware of where they are, others are aware even if they are unable to talk because of intubation.
She brought in a white board for one woman whom most of the hospital workers assumed was checked out and discovered that once the patient had the board she could communicate. “I could hear all of you and you were always nice to me,” the patient told Rapaport via the board.
After she started bringing in supplies to help stimulate patients, she said donations of colored pencils, coloring books, word puzzle books and mini-radios began to arrive. The radios were important because many of the patients couldn’t focus and follow television programs and the music helped stimulate them.
Music during therapy
“I like to play music at each therapy session,” Rappaport said. She calls physical therapist Marcus Jackovitz, with whom she works daily, “her partner in crime.”
“He’s the music man, the one who chose the music for everyone,” she said. “He’s as much a hero as anyone else.”
During a long hospitalizations, Rapaport said, “Things slip through the cracks and I’m trying to seal up the cracks.”
Sometimes patients just need someone to listen to them, she said. “Some patients were so preoccupied with what was going on outside the hospital — their bills, their families — that they couldn’t concentrate on their therapy.” So she has relayed information on relief programs and reassured them until they were able to focus on tasks such as learning to feed and groom themselves again.
Giving patients back their independence is a big part of restoring their quality of life, she said.
“I try to help patients get back to where they were before the pandemic,” she said. “I treated them as I would my family; I thought of them as a parent, a sibling. That’s the way I could do my job.”
Rapaport herself came down with COVID last November at Thanksgiving time. While she wasn’t hospitalized, the 28-year-old said she had a few days where she couldn’t stand up without help.
The pandemic also took a physical and emotional toll on Rapaport at work.
Last spring, when no one was quite sure how transmissible the virus was, therapists working with COVID patients had to wear two gowns, disposable booties that went up to their shins, and hair nets in addition to their masks and face shields or goggles.
Putting on PPE took a half hour, and there were days when Rapaport had to change her scrubs three times because I was “so drenched.” The work was physical because therapists were called upon to turn and move patients.
“We’ve shed a lot of that PPE now,” she said.
Hits hard when you lose a patient
One of the hardest things for Rapaport was evaluating a patient who might be breathing on their own one day and chatting about their dogs’ names and then coming back the next day to find them intubated and unable to talk.
“As therapists, we’re not trained to lose patients like someone who works in the ICU,” Rapaport said. “This past year I’ve lost perhaps 50 patients. Before that it was one.”
So, in late March, she asked to take a break from the COVID unit. She’s now working on training new hires at the hospital but calls stepping away a “temporary pause.” She expects to return to her work with COVID patients.
At Cleveland Clinic Weston, signs posted outside medical buildings read “You are our heroes” and “Thank you Cleveland Clinic caregivers.” They are a constant reminder of just how hard hospital employees have worked to treat COVID patients.
As cases of COVID-19 began to spike in the spring of 2020, stretching staff to their limits, Smith, the hospital’s director of physical therapy, thought it was also important for her team of more than 67 physical therapists, occupational therapists, and athletic trainers to show their colleagues their appreciation and help them “get through the new stresses.”
While the therapists were needed to help rehabilitate COVID-19 patients whose limbs and joints had stiffened after long periods in bed, the hospital’s outpatient therapy numbers had fallen sharply in the early days of the pandemic, mainly because people were afraid to come into a medical facility, Smith said.
Massages, relaxation station
To keep the therapists busy and to help hospital workers exhausted by the pandemic, Smith and her team created a novel “relaxation station” for colleagues within the hospital.
The therapists worked with their hospital colleagues to help them relax and take a quick break at the relaxation station where they could get massages and ease tired and sore legs and feet with foot massagers and pneumatic leg pumps.
Outside donors were so happy with what they were trying to do that they donated numerous items. One vendor supplied Theraguns, which provide deep muscle massage; another lent recovery pump boots and a local store provided foot massagers and other self-care items.
Beginning in late March 2020 when lockdown began until last July, there was a dedicated space within the hospital from 7 a.m. until 9 p.m. where tired hospital employees could find a respite. Sometimes the therapists took the massage equipment to nursing stations or to other Cleveland Clinic locations around South Florida.
To make sure no one was left out, Smith said employees who were repositioned to work from home were also invited to come in for a dose of relaxation.
“We thought this was a really important thing to do for each other,” Smith said. “It was very well-received. The team here at Cleveland Clinic has been amazing to work with through the pandemic.”
Now that the hospital isn’t as overwhelmed as it was at the peak of the pandemic, and as the therapists’ caseloads return to normal, the relaxation station has been disbanded. But Smith said her team is still trying to put on events twice a month to help hospital workers de-stress.
During a recent lunch break, yoga mats were brought outside, and massage guns were made available so workers could do self-massages.
This story was originally published April 29, 2021 at 12:34 PM.