‘Every single mask makes a difference’ as Florida hospitals try to avoid coronavirus shortages
Before the coronavirus, the protective gear doctors and nurses wear was treated as a “one-time thing.”
“In a non-pandemic situation, you go see that patient, you come out of the room and you throw the mask away,” said Dr. Jennifer Jackson, a professor at the University of Miami medical school.
Now, medical providers in hard-hit places like New York wear masks for a week straight, wiping them down with hand sanitizer in between patients. Even in Florida, which on Thursday surpassed 8,000 cases, doctors and nurses have been told to wear a single mask for a 12-hour shift.
Some of that comes at the explicit approval of the Centers for Disease Control and Prevention, which released guidelines on “extended use” and “reuse” of a single mask as the rapid-fire spread of COVID-19 strains the national healthcare system.
While the CDC policy may stretch a dwindling supply, it’s freaked out medical professionals around the country who worry they’re not being properly protected. Some have taken to social media to voice their fears under the hashtag #GetMePPE, which stands for personal protective equipment — PPE for short.
National Nurses United, which represents Florida nurses around the state, organized protests after its members reported some Florida hospitals barred nurses from bringing their own protective gear, even sending them home when they showed up with an N95 mask.
The PPE shortage, or fear of a future one, has driven Miami medical professionals to unusual lengths. University of Miami medical school students organized a phone bank soliciting donations from local businesses. Jackson Memorial Hospital residents organized a GoFundMe. Broward Health’s fundraising arm has pivoted to collecting cash for more PPE.
One Miami doctor is even working with doctors and researchers across the world to adapt a full-face snorkel mask for diving into medical protective gear.
With cases of COVID-19 climbing in South Florida, the hot spot of the Sunshine State, some hospitals have begun handing out protective gear to more and more staff members, not just those working directly with coronavirus patients.
“The philosophy of assuming everyone is COVID positive keeps patients and providers safe,” said Jackson, an emergency medicine physician. “We’ve seen so many patients that are there for something completely different than COVID, then while they’re there, they’re tested and come back positive.”
That kind of culture prevents transmission of the virus, but it also means hospitals run through a lot of masks, which are getting harder and harder to replenish. And the government is only so helpful.
The Strategic National Stockpile has millions of masks and other equipment in emergency reserve at secret storerooms to prevent theft. Florida is one of the few states that has had its requests filled by the federal government, although officials told the Washington Post that stockpile is now nearly depleted. But Florida hospitals need more than the two million N95 masks, half a million gowns and gloves and 150,000 PPE protection kits delivered on a continuing basis.
Jared Moskowitz, director of the Florida Division of Emergency Management, went on Twitter Monday to ask 3M to send N95 masks directly to hospitals, first responders and his division to avoid scams and price-gouging.
“How many brokers and distributors do we have to negotiate with only to find empty warehouses?” he asked.
3M tweeted back that it is doubling its global production to 100 million per month.
Then Mark Cuban, owner of the NBA’s Dallas Mavericks and a star on the “Shark Tank” TV series, chimed in. He has said 3M’s distributors and resellers are bidding up prices to take advantage of demand.
Moskowitz responded to Cuban that “it feels like a Ponzi scheme. Different distributors represented by brokers selling the same lot of masks bidding against each other. I’m chasing ghosts here.”
Nonprofits, like the Broward Health Foundation, the fundraising arm of Broward Health, are running into similar roadblocks.
“The prices are exorbitant in regard of what we used to pay. Four and five times as high,” said Bill Diggs, president of the Broward Health Foundation. “We used to get stuff in seven to eight days. And now it takes much longer.”
That means the foundation needs more money than usual to outrun the shortages and stock up before South Florida hits its peak of COVID-19 cases, something some models have pegged for the beginning of May.
The foundation is reaching out to its usual donors, but also asking members of the public to pitch in what they can, no matter how small.
“If they’ve got two masks, we’ll take ‘em,” he said. “Listen, we’ll take five bucks.”
The foundation is also collecting iPads and tablets so that hospitalized COVID-19 patients, who aren’t allowed visitors, can video chat with loved ones.
Diggs, a longtime fund-raiser, said this is the most important cause he’s ever worked for, because protecting front-line healthcare workers is the only way to prevent a collapse of the nation’s healthcare system.
“That community is finite — you and I cannot go and replace them. We can’t,” he said. “If we can’t keep them safe, the bottom really does fall out.”
UM medical school students started their own effort after their class schedule dissolved into online lectures. Around a hundred students organized and started offering what help they could to doctors and nurses on the front line, like child care and meal delivery.
They connected with medical students in New York, who shared a unique strategy. They used a computer program to scrape data off Yelp and compile a list of businesses that might have extra protective gear to donate, like tattoo parlors, nail salons and hardware stores.
Students arranged a phone bank to call those businesses and ask for donations. Alison Ohringer, the class president of UM’s first-year medical school students and leader of the effort, said donors often feel like their contribution is too small. But she said even a handful of masks is a big deal.
“People ask, ‘Are you sure? I just have three.’ The answer is absolutely yes, because every single mask makes a difference,” she said. “People on the front line of this pandemic are given one mask that they have to use until it disintegrates.”
Donors drop off their contributions at her apartment and student volunteers take it to whoever needs it. So far, Ohringer said her team has donated to three Miami hospitals and plans to expand to even more medical centers in the coming weeks.
In a little over a week, the UM students have gathered thousands of pairs of gloves and face shields and more than a hundred N95 masks, as well as hundreds of appreciation cards for stressed-out healthcare workers.
Residents at Jackson Memorial Hospital put together a GoFundMe to raise $9,000 for PPE — a goal they surpassed in less than a week. A couple of days after the fundraiser went live online, it dropped the hospital name; “this was a request,” the description said.
As everyone in the medical community desperately scrambles to stockpile protective gear, some have started to plan for a future where those basics aren’t available.
At the University of Florida Health, an anesthesiologist is experimenting with creating masks out of the sterile fabric used to protect surgical equipment.
Dr. Roberto Miki, a hand surgeon with the University of Miami, is working with doctors around the world to perfect another possible solution.
Because the work he does isn’t explicitly with coronavirus patients, he said he isn’t given one of the hospital’s rationed N95 masks. But with so many COVID-19 patients not showing symptoms and a lack of testing to show how widespread the virus actually is, Miki said he didn’t want to take chances. So he wears his own personal N95 with a surgical mask on top of it.
“You have to assume everyone has it,” he said.
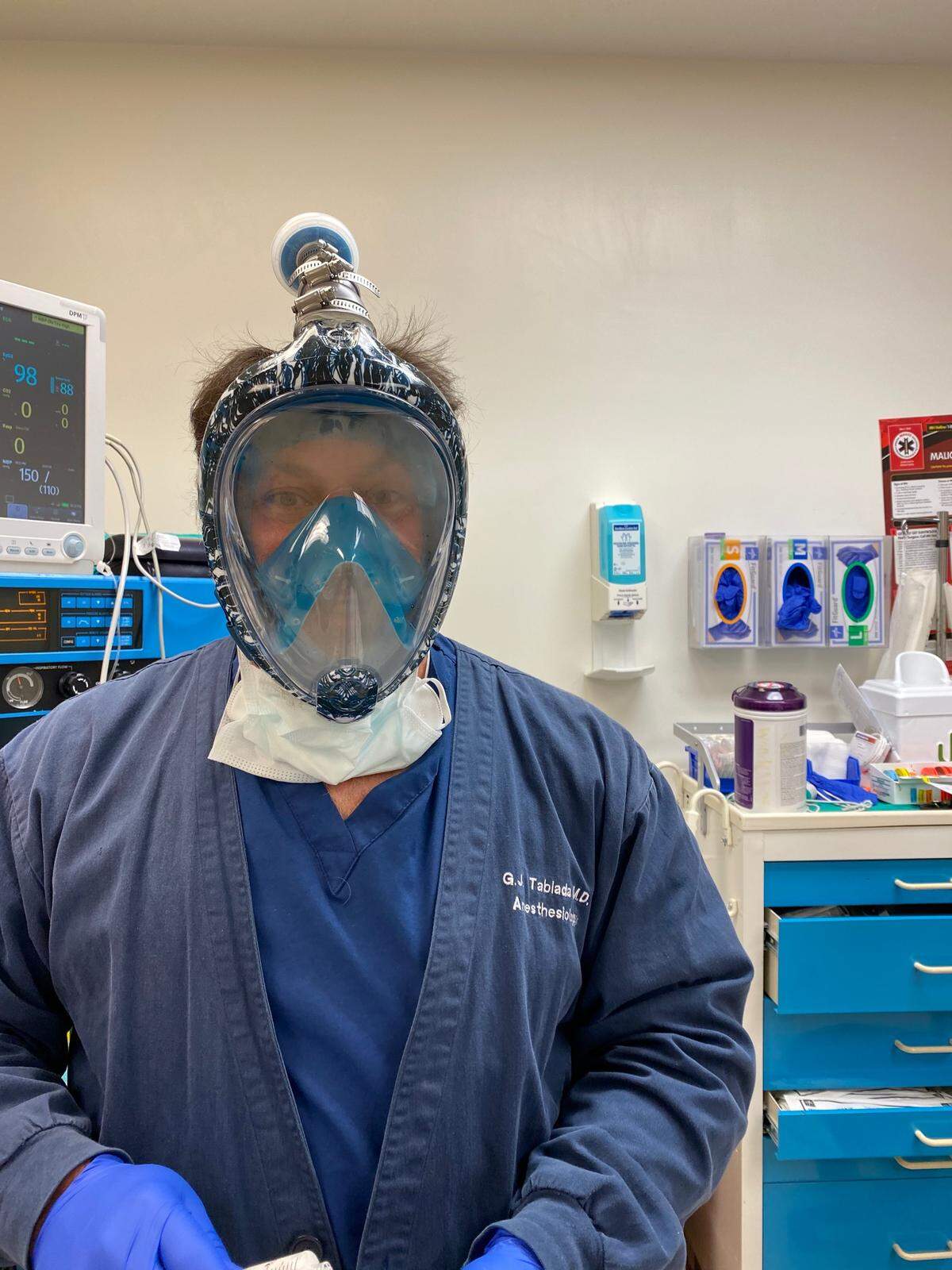
He expects those to run out eventually though, so he’s experimenting with another option — a full-face snorkel mask with a medical-grade air filter at the top. It’s especially important for Miki because his wife has severe asthma, so a respiratory illness like COVID-19 would be devastating.
“I needed to figure out a way to protect her from me,” he said. “It’s not if they’re going to run out of PPE, it’s when.”
He’s already living in a spare room in the house, sealed off from his family. He attended his child’s birthday the other day via Zoom and only interacts with his family on FaceTime.
That’s given him plenty of time to tinker. Miki posted a YouTube video explaining his process with the snorkel mask and immediately received dozens of emails pointing him toward people around the world who came up with the same idea. Researchers at Stanford University in California submitted a similar application for FDA approval.
Before long, he was on Zoom calls with doctors from Italy, New York, the University of Michigan and Stanford, all working on perfecting this mask. They’re also working collaboratively on a Google Doc with constantly updating best practices.
The University of Michigan bought 4,000 of these masks, he said, as a backstop against other shortages. Miki has talked to administrators at the University of Miami and Baptist Health about potentially using the masks, but he said they’ve been skeptical.
“They feel reluctant to use it because it’s not an FDA approved option,” he said. “It’s not FDA approved, but it’s your last line.”
Without FDA approval, it’s unlikely any hospital would consider an unproven substitution for an N95 mask. But if things get more dire in Florida, like they are in New York, Miki said it’s likely South Florida practitioners will start using whatever they can find to keep themselves safe.
“Some of them are going to use it even if they don’t have permission,” Miki said. “It’s my personal N95. I’ll take the risk. Anybody who’d give them a hard time has no leg to stand on.”
Miki submitted plans for his own adaptor to a local 3D printing company, 3DChimera, which is now selling an optimized version for $10. Full face masks run around $40, he said, and the filters are relatively cheap too. Although they’ve jumped from $2 each to $6 each recently.
Alexander Hussain, head of Miami-based 3DChimera, got into the business of printing medical devices when his brother, a doctor in Tampa, called him for help.
“He said the hospital asked people to develop their own equipment. I thought that was crazy,” Hussain said.
So his team came up with a design for a face shield and started printing 24/7. They were quickly overwhelmed with orders. They’re dropping off dozens to local hospitals, like Mount Sinai, Jackson Memorial and South Miami, daily. Miami-Dade Police and Fire Rescue have also placed orders.
The face shields go for $20 and print in about three hours. Under normal circumstances, Hussain said, a print job like that would run a customer $200. The company is also offering a deal where for every piece of gear purchased they donate another one to a hospital in need.
“We’re super happy to help,” he said. “But it is pretty mind-blowing to us that doctors, nurses, police and fire are taking it upon themselves to buy their own gear because their organizations can’t find a solution.”
What’s most frustrating for Hussain is how inefficient the process is. His six printer setup can make 30 or so masks a day, but if they were supporting a bigger company with more industrial ability, they could up their output considerably.
“We can spend 100 hours making a machine that can make 1,000 masks an hour, or we can spend 1,000 hours making 100 masks,” he said.
To donate to the University of Miami student effort, visit www.miamimedcovidhelp.com/donate.
The Broward Health Foundation is accepting donations at BrowardHealthFoundation.org or by phone at 954-712-3980.
Miami Herald staff writer Linda Robertson contributed to this report.
This story was originally published April 2, 2020 at 12:37 PM.
