New study shows potential link between bad quality sleep and Alzheimer’s in Hispanics
Hispanics who have trouble sleeping may be at a higher risk of Alzheimer’s disease or other dementias, according to a new study.
The study found a possible link between insomnia, prolonged sleep duration (more than nine hours of sleep) and a decline in neurocognitive functioning, which could precede Alzheimer’s disease or other dementias, said Dr. Alberto R. Ramos, the lead author of the study and an associate professor of neurology at the University of Miami’s Miller School.
“This finding is particularly important because Hispanics have a significantly higher risk of Alzheimer’s disease compared with non-Hispanic whites,” Ramos said.
Alzheimer’s, one of the most common types of dementia, is one of the top 10 leading causes of death in the United States and is the fifth most common cause of death for Americans 65 and older, according to the Centers for Disease Control and Prevention.
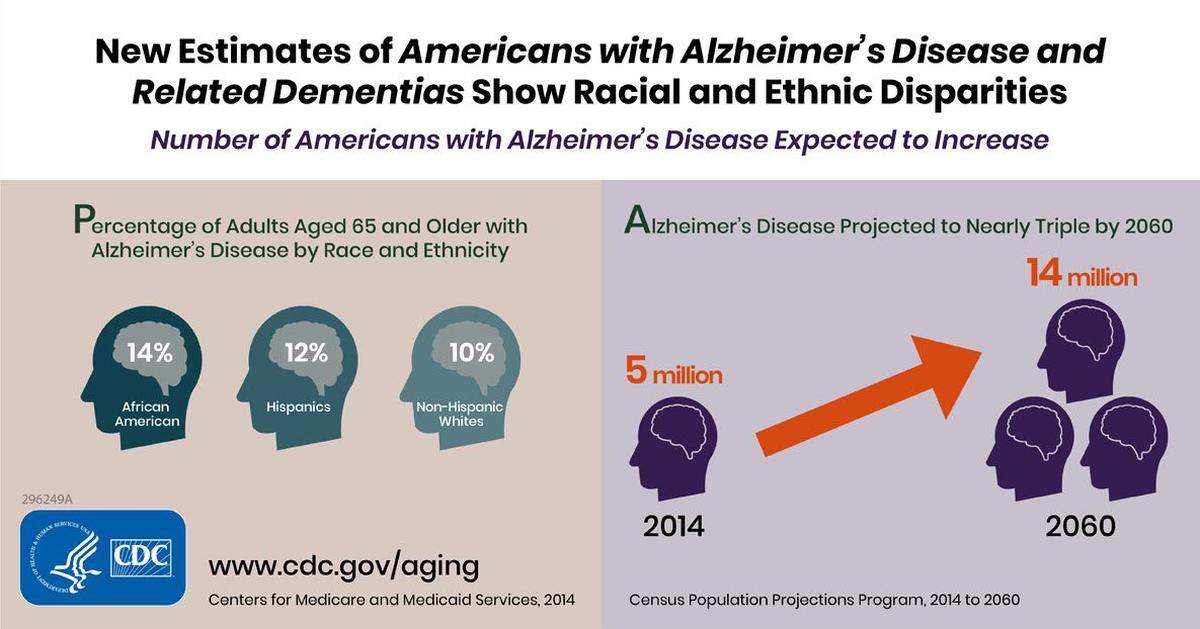
More than five million people had Alzheimer’s or another dementia in 2014, and the center expects these numbers will double by 2060. Hispanics, the country’s second-fastest growing racial or ethnic group, are projected to have the largest increase of Alzheimer’s or other dementia cases, according to a 2018 CDC study.
While non-Hispanic whites will still have the largest total numbers of Alzheimer cases, the center says African Americans and Hispanics have a higher risk of getting diagnosed with Alzheimer’s disease and related dementias. By 2060, the center estimates there will be 3.2 million Hispanics and 2.2 million African Americans affected by the disease.
Ramos hopes the study he and his team are working on will open the door for new discoveries and possibly a solution on how to prevent dementia.
During his study, researchers across the country analyzed a variety of sleep disturbances including sleep apnea — which has been linked to impaired cognition — among 16,000 Latinos from diverse backgrounds at four urban centers in Chicago, Miami, San Diego and the Bronx in New York City.
The participants were selected from the nationwide Hispanic Community Health Study/Study of Latinos, which is considered by researchers to be the most comprehensive study of Hispanic/Latino adults in the United States. The largest groups were Central American, Cuban, Dominican, Mexican, Puerto Rican and South American. Fifty-five percent were women.
Later, 5,247 people between 45 and 75 years old were selected to represent the “snapshot” of U.S. Latinos in the study, said Ramos.
“No previous studies used data from a representative sample of U.S. Hispanic/Latinos for these multiple types of sleep disturbances,” he said.
.jpg)
During the study, participants were given a neurocognitive test, which examined their mental status, verbal episodic learning and memory, word and verbal fluency and their processing speed. Seven years later, they were tested again.
“We observed that prolonged periods of sleep and chronic insomnia symptoms led to declines in memory, executive function and processing speed,” said Ramos. “Those measures can precede the development of mild cognitive impairment and Alzheimer’s disease.”
Insomnia affected memory more while abnormal periods of sleep affected executive functions and processing speed, which is how the mind organizes and understand information, he said.
While those who slept less than six hours did not see a decline in episodic learning and memory, Ramos said they’re more vulnerable to other health problems like high blood pressure and obesity.
Ramos said it’s still too early to tell, at this point in the ongoing study, who will be diagnosed with symptoms of Alzheimer’s or dementia. But, he said the findings are a good indicator of vulnerability.

The neurologist also said the study will provide a foundation for building awareness among physicians that sleep disturbances may be linked to neurocognitive decline, particularly among Hispanic patients.
“We may also be able to identify at-risk patients who may benefit from early intervention to prevent or reduce the risk of dementia,” he said.
Ramos also hopes the study will help influence a “change of culture” and remind people that just like dieting and exercising, the right amount of sleep is important for your health. For adults, the “sweet spot” is seven to nine hours of sleep, he said.
The study “Sleep and Neurocognitive Decline in the Hispanic Community Health Study / Study of Latinos” was published Wednesday in Alzheimer’s & Dementia: The Journal of the Alzheimer’s Association.
This story was originally published October 9, 2019 at 11:22 AM.
