Treating diabetics’ wounds is critical to long-term outcome of patient
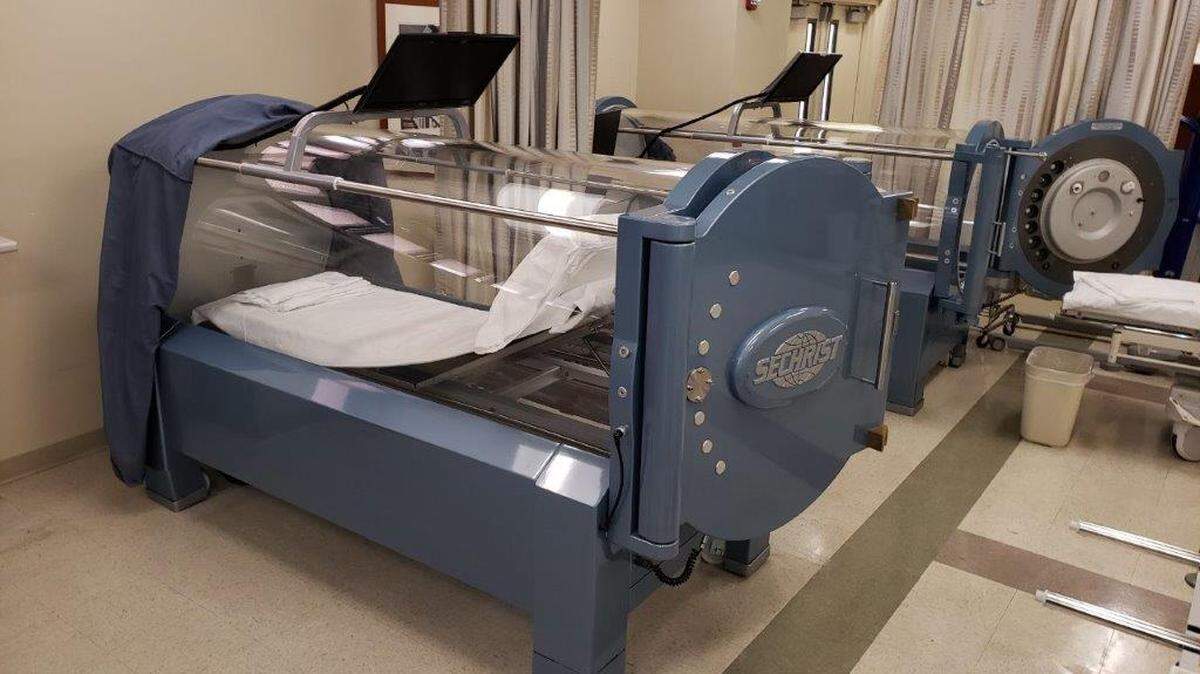
Alma Reyes, who has been living with diabetes for nearly a quarter-century, admitted she was “very scared” when she first agreed to undergo hyperbaric oxygen therapy, also known as HBOT.
But Reyes, 52, believes the treatment she received at South Miami Hospital saved her right foot from at least partial amputation. She had gotten hurt when she stepped on a rock without wearing proper shoes. Within three days, her foot had swollen and had become infected.
“It looked like a balloon,” she said. “If I had waited another 24 hours to go to the hospital, they would have had no choice but to amputate.”
Instead, doctors employed HBOT, which is often used on diabetic patients to treat wounds, a common problem for diabetics, especially foot wounds. The therapy pumps an elevated supply of oxygen into a patient’s lungs — about three times the normal amount — which is then dispersed throughout the body through the blood, according to the Mayo Clinic.
The extra oxygen releases stem cells that help the body heal. When the body’s tissues are injured, they need even more oxygen to survive and ward off infections.
“Going to the hospital is normally a nightmare for me,” Reyes said. “But this therapy was actually very calming, and my wound healed very quickly. I was not even halfway through the treatment when they said I was completely healed.”
HBOT is not new technology, but it’s been increasingly used in treating wounds. Oxygen therapy initially was used to treat air bubbles caught in your blood vessels, a condition that can develop from scuba diving. Today, it’s used for treating serious infections, in addition to wounds.
Here’s how the therapy works: The chamber delivers 100 percent oxygen at a pressure that is greater than atmospheric. Wounds need oxygen to heal. Thus, exposing a patient to 100 percent oxygen can speed up the healing process.
Oxygen is also vital for the production of collagen, a protein that strengthens your skin and bones.
In addition, HBOT has been found to have an anti-microbial effect, which allows white blood cells to fight infection.
Wounds and diabetics
Wounds are a serious issue for diabetics.
About 30 million Americans have diabetes, and 1 out of every 4 will experience a foot ulcer. Statistics show that 15 percent of diabetic foot ulcers progress to amputation, and 50 percent will die within five years of an amputation. Furthermore, 40 percent of people with a healed foot ulcer will develop a new ulcer within a year.
Adrian Diaz, the clinical program director for Hialeah Hospital’s Center for Wound Care and Hyperbaric Medicine, said wound-care centers exist to provide advanced treatment for chronic, non-healing ulcers that could otherwise lead to amputation.
One of Diaz’s patients, Dino Engram, was a diabetic with a foot ulcer and a bone infection. Another hospital had recommended amputation, but Engram sought a second opinion at Hialeah Hospital.
Dr. Sandra L. Franco and her team cleaned the infection surgically and used a total-contact cast, saving his leg. They also used a wound vacuum to remove the wound’s excess fluid.
“The patient had developed a flesh-eating bacteria, which can be deadly,” Franco said. “We were able to save his life and his leg by applying negative-pressure wound therapy, which functions like a vacuum cleaner, draining fluid to promote healing.”
Franco said the total-contact cast was used to keep Engram from walking on his wound. If a patient continues to walk on his or her wound, healing will not occur. Although work still remains, Engram’s wound has been 90 percent resolved.
“The original wound covered 60 percent of his foot,” Franco said. “Now, the wound is about the size of a quarter.”
Avoiding complications
For many people with diabetes, the chances of developing additional complications such as peripheral vascular disease, also known as PVD, is far more likely than the general population.
PVD, which affects blood vessels outside the brain and heart, can increase the likelihood of strokes, heart attacks and limb amputations.
Mount Sinai Medical Center in Miami Beach has a limb-salvage program that uses high-resolution technology to treat wounds.
“We’re able to restore blood flow,” said Dr. Timothy Yates, a radiologist at Mount Sinai. “The goal is to open blocked blood vessels in the legs, feet, and toes.”

Using high-resolution imaging and the latest technology, interventional radiologists are able to perform the majority of procedures using a special needle, with no incisions or open surgery. Most patients return home the same day of the procedure.
Dr. Brandon Olivieri, part of Mount Sinai’s team of vascular and interventional radiologists, said diabetes is the leading cause of limb amputation, and that’s a result doctors battle to avoid.
“The reason we take this so seriously is that once a patient loses his or her leg they often lose the will to live,” said Dr. Robert Beasley, chief of vascular and interventional radiology at Mount Sinai. “That’s why we fight so hard to save limbs. We have a saying, ‘Save a limb, save a life.’’’
This story was originally published November 20, 2018 at 7:00 AM with the headline "Treating diabetics’ wounds is critical to long-term outcome of patient."